For many years, women with endometriosis have faced a frustrating reality: severe symptoms, years of uncertainty, and a diagnosis that often required surgery to confirm. The new clinical guidance from the American College of Obstetricians and Gynecologists (ACOG) signals an important shift in how this disease is recognized and diagnosed. The goal is simple but powerful—shorten the time to diagnosis and begin treatment earlier.¹
As someone who has spent decades caring for women with pelvic pain, infertility, and hormonal disorders, I find these changes both encouraging and long overdue. They reflect what many clinicians have observed in practice for years: endometriosis is often clinically obvious long before it is surgically confirmed.

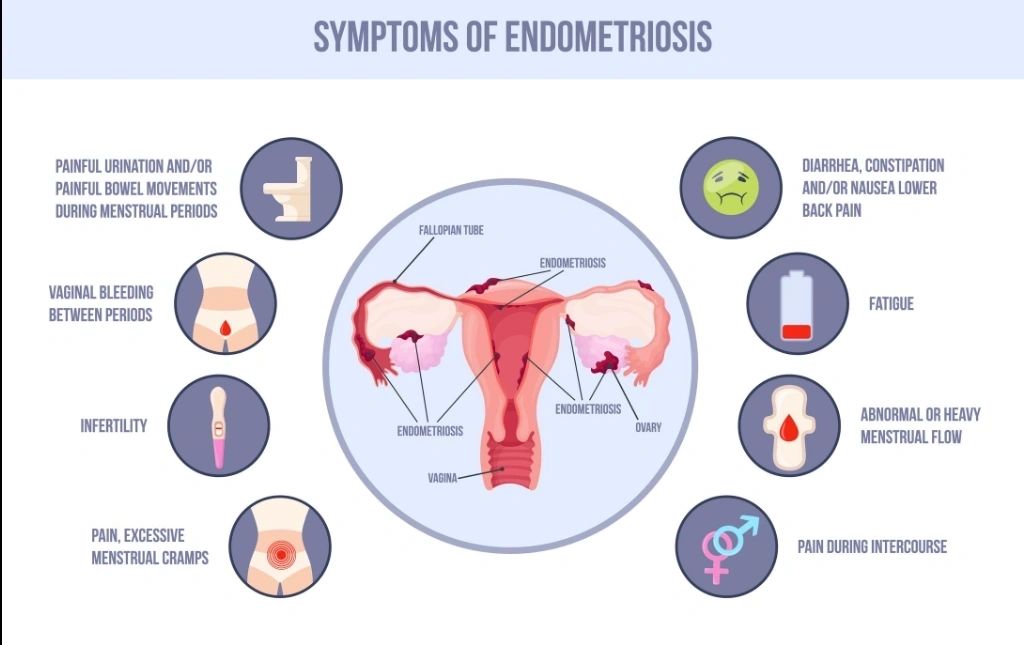
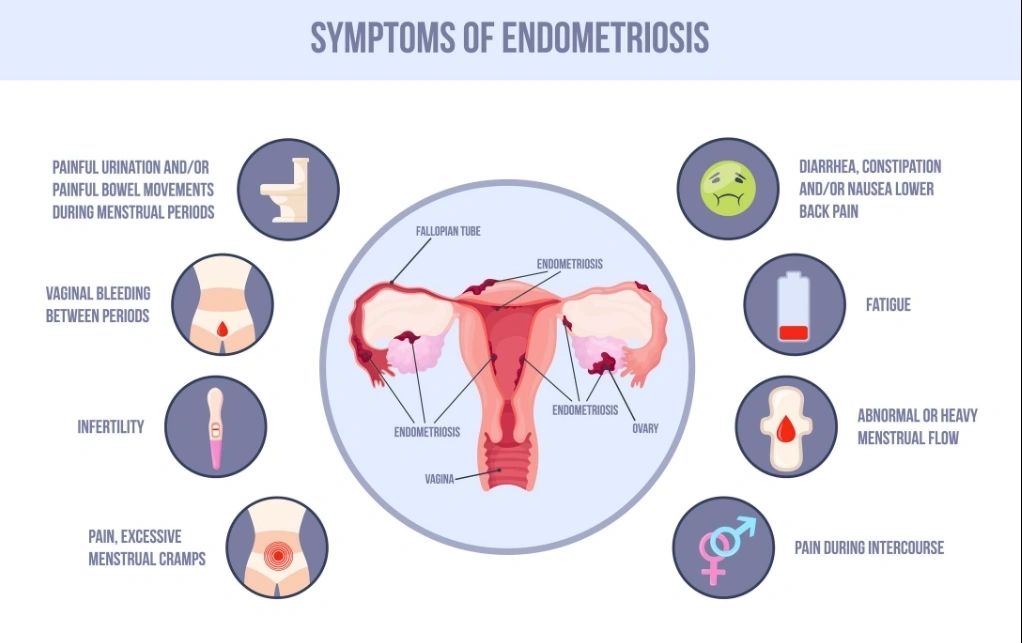
Endometriosis is a chronic inflammatory condition in which tissue similar to the uterine lining grows outside the uterus. It can cause severe pelvic pain, painful periods, pain with intercourse, bowel or bladder symptoms, and infertility.²
Despite affecting roughly one in ten women of reproductive age, diagnosis has historically been delayed. On average, women wait four to eleven years from the onset of symptoms before receiving a definitive diagnosis.¹,³
There are several reasons for this delay:
- Historically, laparoscopy with biopsy was considered the gold standard for diagnosis.
- Many symptoms overlap with other conditions, such as irritable bowel syndrome or pelvic floor disorders.
- Women’s pain has often been dismissed or normalized, particularly in adolescents and young adults.
- Limited awareness among clinicians outside gynecology can delay referral and evaluation.¹
The result is that many women suffer for years before receiving appropriate care.
The most significant change in the new ACOG guidance is that endometriosis can now be diagnosed clinically, based on symptoms, examination findings, and imaging—without requiring surgery for confirmation.¹
In practical terms, this means physicians are encouraged to:
- Recognize common symptoms such as
- dysmenorrhea
- chronic pelvic pain
- deep dyspareunia
- bowel or bladder pain
- infertility associated with pelvic pain
- Use pelvic examination and imaging, particularly transvaginal ultrasound, as part of the evaluation.¹
- Consider MRI for more complex disease.¹
- Begin empiric treatment when clinical suspicion is high.³
Laparoscopy remains valuable—especially when imaging is inconclusive, or surgery is planned—but it is no longer required simply to make the diagnosis.
One of the biggest advantages of this approach is that treatment does not need to wait for surgery. Women can begin therapies that reduce inflammation, suppress endometrial activity, and relieve pain while evaluation continues.¹
By allowing clinicians to make a presumptive diagnosis, these guidelines aim to shorten the diagnostic journey that has historically lasted nearly a decade for many patients.¹,³
Earlier recognition may also benefit women trying to conceive. Endometriosis is strongly associated with infertility, and earlier diagnosis can guide fertility planning and treatment decisions.²
The guidelines emphasize shared decision-making, acknowledging that patients should participate actively in choosing diagnostic and treatment pathways.¹
Importantly, the new guidance highlights how racial bias and gender identity bias can delay diagnosis and treatment, calling for improved education and more equitable access to care.¹
From a clinical perspective, these recommendations align with a broader trend in medicine: moving from invasive diagnostics toward symptom-based and imaging-based evaluation whenever possible.
For patients, the message is equally important:
- Severe menstrual pain is not normal.
- Persistent pelvic pain deserves investigation.
- Women should feel empowered to seek a second opinion if symptoms are dismissed.
For clinicians, the guidelines reinforce something I have often told my patients: listen carefully to the story the patient is telling you. In many cases, the pattern of symptoms already points strongly toward endometriosis.
The shift toward clinical diagnosis is only the beginning. Endometriosis research is rapidly evolving, with growing recognition that the disease involves complex interactions between immune, inflammatory, hormonal, and environmental factors.
As our understanding improves, we may see:
- earlier screening strategies
- improved imaging techniques
- personalized treatment approaches
- greater integration of lifestyle and metabolic health in management
For women who have struggled for years to have their pain recognized, these new guidelines represent something important: progress.
And progress, in medicine, often begins with simply believing what patients have been telling us all along.
A Final Thought
For too long, many women with endometriosis have been told that severe menstrual pain is “normal.” It is not. The new ACOG guidelines represent an important step forward in recognizing symptoms earlier and reducing years of unnecessary suffering.
Understanding how lifestyle, hormones, inflammation, and metabolic health influence reproductive health is also an essential part of the conversation.
If you would like to learn more about protecting and optimizing your fertility, my new book Optimize Your Fertility Naturally explores the science behind reproductive health and practical strategies women can begin using today.
My ebook is now on a prelaunch SALE:
https://www.amazon.ca/Optimize-Your-Fertility-Naturally-Achieving-ebook/dp/B0GQJ6BM64
Because fertility is not something we should think about only when there is a problem. It is something worth protecting long before that.
- American College of Obstetricians and Gynecologists. “Diagnosis of Endometriosis.” ACOG Clinical Practice Guideline No. 11. Obstetrics & Gynecology 147, no. 3 (2026).
- American College of Obstetricians and Gynecologists. “Endometriosis.” ACOG Frequently Asked Questions.
- American College of Obstetricians and Gynecologists. “ACOG Publishes New Endometriosis Clinical Guidance Aiming to Shorten Time to Diagnosis and Improve Access to Care.” 2026.
- Pelc, Corrie. “New ACOG Guidelines May Help Change, Shorten Endometriosis Diagnosis Times.” Medical News Today, 2026.
Dr Marina OBGYN