For three decades, I’ve sat across from women at every stage of their reproductive lives — medical students in their twenties, professionals in their thirties, and women in their forties who assumed they still had time. The question I hear most often now is not “Can I get pregnant?” but “When should I freeze my eggs?”
Egg freezing has quietly shifted from a niche fertility procedure into a cultural milestone — a kind of biological insurance policy. But like any form of insurance, its real value depends entirely on when you purchase it, why you’re doing it, and what you understand about the fine print.
Let’s replace fear with a framework.
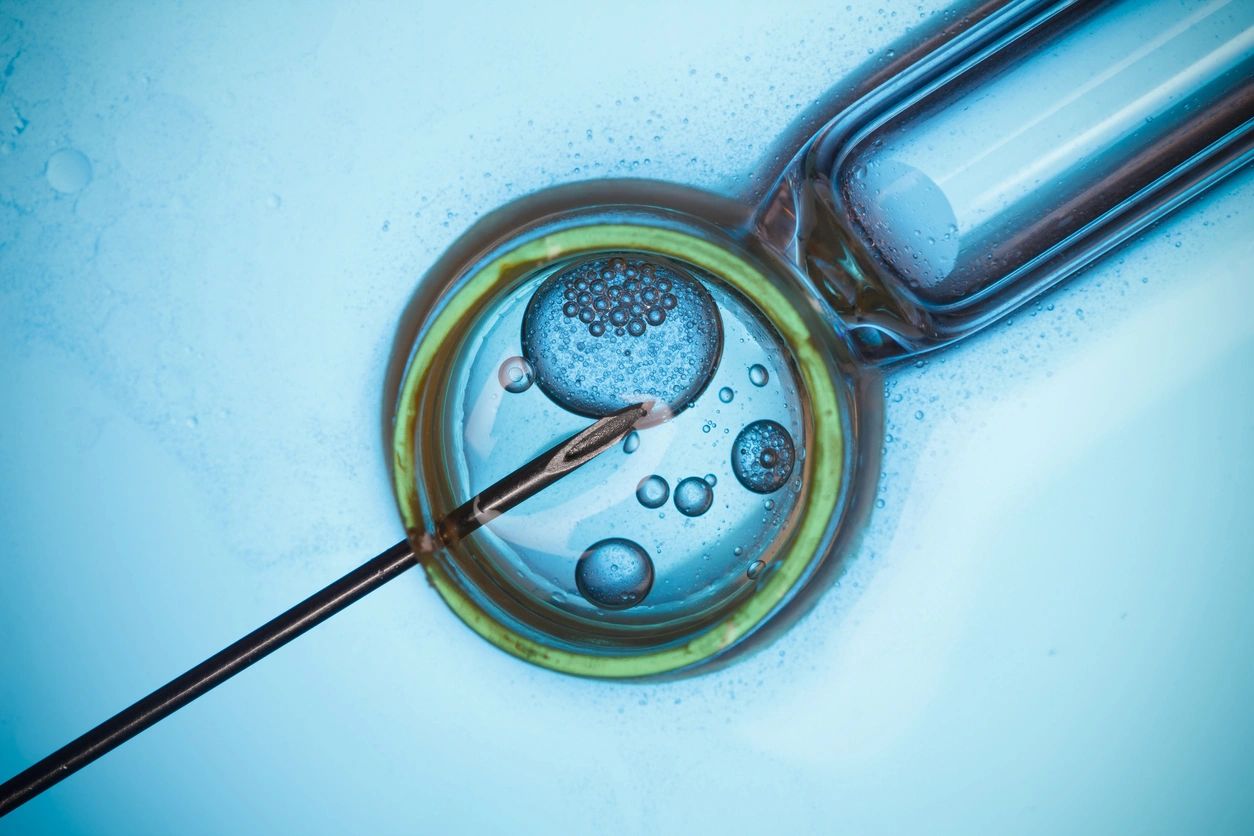
Women are born with all the eggs they will ever have. Over time, both quantity and quality decline, but not at the same pace for everyone. This is where lifestyle can account for differences. What changes most dramatically with age is not just how many eggs remain — it’s how many of those eggs are genetically capable of becoming healthy embryos.
By the mid-30s, the risk of chromosomal abnormalities rises sharply. By the early 40s, even when eggs are retrieved, a much smaller percentage will lead to viable embryos. This is why freezing younger eggs often translates into a higher chance of future success — not because pregnancy becomes impossible later, but because the biological odds quietly shift.
At this stage, egg quality is typically excellent. From a purely biological perspective, this is the most efficient time to freeze.
But biology is only part of the equation.
Women in their twenties are often still defining careers, relationships, geography, and financial stability. For some, egg freezing offers peace of mind — a psychological buffer against life’s unpredictability. For others, it can feel like solving a problem they may never have.
Clinical reality:
Fewer eggs are usually needed at this age to achieve a future pregnancy, which can mean fewer stimulation cycles and lower long-term costs. But it’s also the age when many women may never need to use what they freeze.
This is the age I often describe as the crossroads.
Fertility is still present. Egg quality is still reasonable. But the decline is no longer theoretical — it’s measurable. Anti-Müllerian hormone (AMH) levels, antral follicle counts, and cycle regularity begin to tell a clearer story about where the ovaries are heading.
This is often the moment when women freeze eggs not out of abstract planning, but out of real-world awareness — a career that took longer than expected, a relationship that hasn’t yet become a family, or personal circumstances that made timing unpredictable.
Clinical reality:
More eggs are typically needed at this age to create the same future pregnancy potential as someone in their late twenties. The technology still works well — but efficiency is no longer guaranteed.
By forty, egg freezing becomes less about insurance and more about informed probability.
It can still be done. And for some women, it makes sense — particularly if ovarian reserve is better than expected or if there is a strong personal or medical reason to try. But success rates are lower, and multiple cycles are often required to store a meaningful number of eggs.
This is where honesty matters most.
Clinical reality:
Freezing eggs at this stage does not “stop the clock.” It simply preserves a smaller, more fragile set of biological possibilities. For some, donor eggs or embryo creation may ultimately offer higher chances of success.
Rather than asking, “What’s the right age?” I encourage women to ask three better questions:
This includes antral follicle count, cycle history, and — just as importantly — family history of early menopause or fertility challenges.
Career plans, relationship stability, geography, finances, and emotional readiness all matter as much as biology.
This question often reveals the real answer.
Egg freezing preserves potential, not certainty. A frozen egg is not a frozen baby. It is a chance — one that improves with younger age, good ovarian response, and realistic expectations.
What it can offer is time without pressure — time to build a career, find a partner, heal from loss, or simply grow into the life you envision.
I don’t see egg freezing as a symbol of panic. I see it as part of a larger shift — women finally being invited into the biological conversation about their own bodies, rather than discovering the limits only when they reach them.
The real empowerment is not in freezing early or late.
It’s in deciding deliberately.
- American Society for Reproductive Medicine. “Mature Oocyte Cryopreservation: A Guideline.” Fertility and Sterility 99, no. 1 (2013): 37–43. https://doi.org/10.1016/j.fertnstert.2012.09.028.
- Doyle, J. O., S. Richter, M. Lim, et al. “Successful Elective and Medically Indicated Oocyte Vitrification and Warming for Autologous In Vitro Fertilization, with Predicted Birth Probabilities for Fertility Preservation According to Number of Cryopreserved Oocytes and Age at Retrieval.” Fertility and Sterility 105, no. 2 (2016): 459–466.e2. https://doi.org/10.1016/j.fertnstert.2015.10.026.
- Cobo, A., J. García-Velasco, D. Domingo, et al. “Elective and Onco-Fertility Preservation: Factors Related to IVF Outcomes.” Human Reproduction 33, no. 12 (2018): 2222–2231. https://doi.org/10.1093/humrep/dey321.
- Broer, S. L., D. Mol, E. A. Hendriks, and B. C. J. M. Fauser. “The Role of Anti-Müllerian Hormone in Prediction of Outcome After IVF: Comparison with the Antral Follicle Count.” Fertility and Sterility 99, no. 3 (2013): 799–806. https://doi.org/10.1016/j.fertnstert.2012.10.033.
- Goldman, R. H., C. Racowsky, L. V. Farland, S. Munné, L. Ribustello, and J. H. Fox. “Predicting the Likelihood of Live Birth for Elective Oocyte Cryopreservation: A Counseling Tool for Physicians and Patients.” Human Reproduction 32, no. 4 (2017): 853–859. https://doi.org/10.1093/humrep/dex008
Dr Marina OBGYN